- Research
- 2022-2026 Research Strategy
- Open Clinical Trials
- Closed Clinical Trials
- What is a Clinical Trial?
- Why Participate in a Clinical Trial
- Remote Telehealth Pre-Screening Process
- Research Achievements
- Publications
- Research Development and Funding
- Participating Institutions
- International Collaboration
- BCT Trials & Projects Summary
- Translational Research
- Clinical Fellowship Program
- International Fellowship Support
- Annual Scientific Meeting
- Travel Grants and Awards
- About
- Our Impact
- Fundraise
- Donate
- Researcher Login
- Cart
Breast Cancer: The Most Common Cancer Among Women
The World Health Organisation estimates that more than 2.3 million people are diagnosed with breast cancer globally each year. In Australia and New Zealand (Aotearoa), it is the most commonly diagnosed cancer in women.
While more people are being diagnosed with breast cancer each year, thanks to improved screening techniques and treatments, less people are dying from the disease. Without clinical trials research, such as that conducted by Breast Cancer Trials, this wouldn’t be possible.
Download our Breast Cancer Statistics Infographic.
Breast Cancer Statistics for Australia and New Zealand
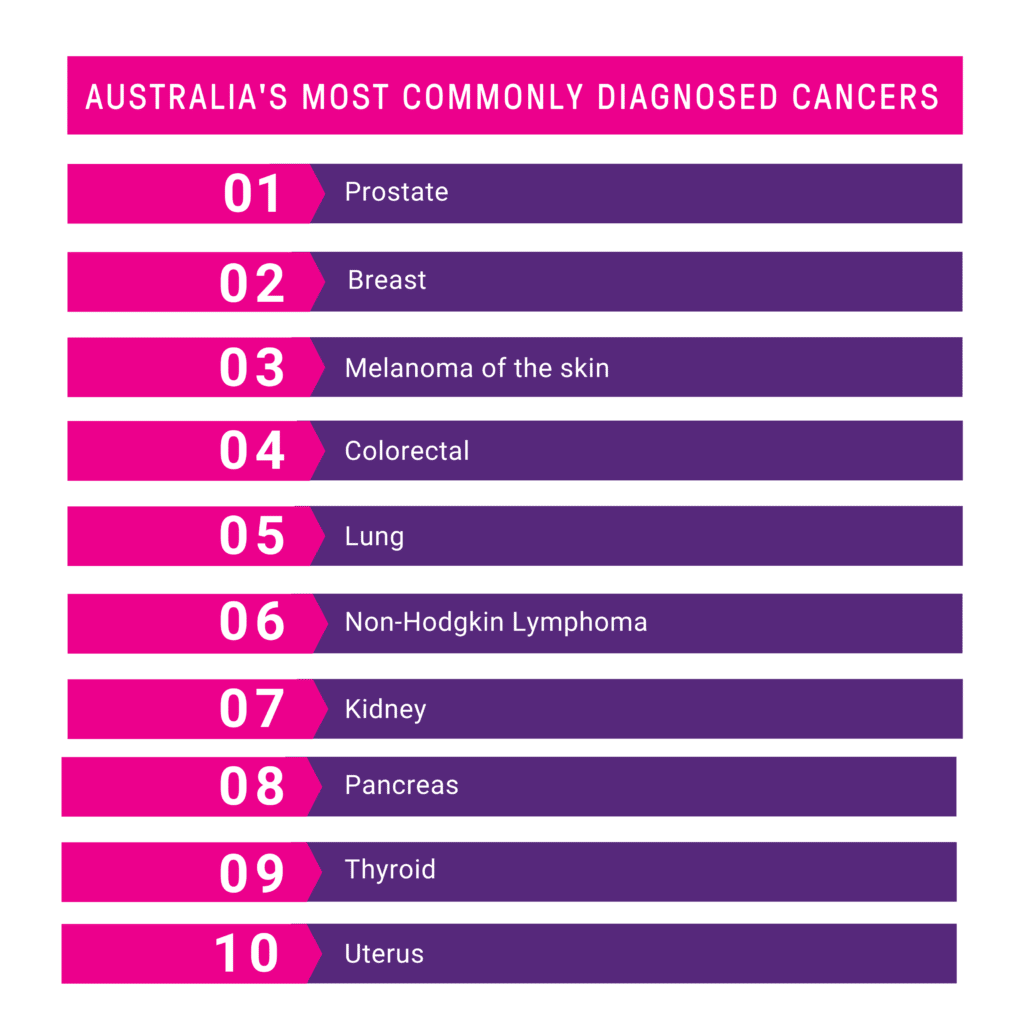
Prevalence of Cancer in Australia
It is estimated that more than 20,440 people in Australia will be diagnosed with breast cancer in 2025, which is 56 people each day. While the prevalence of breast cancer in Australia is increasing, more people than ever are surviving their disease and clinical trials research has played a significant role in this improvement.
Prevalence of Metastatic Breast Cancer in Australia
For the first time, data shows that 20,950 Australians (20,800 women and 150 men) are living with metastatic breast cancer. This figure is double previous estimates and exposes the scale of need and urgency for health system reform.
The Australian Institute of Health and Welfare (AIHW) has released a national estimate that fills a long-standing gap in Australia’s understanding. Until now, there has been no accurate measure of how many people are living with metastatic breast cancer between initial diagnosis and death – a void that has kept thousands invisible in our health system. Below is a state-by-state breakdown of the prevalence of metastatic breast cancer for women in Australia:
- New South Wales: 5,900
- Victoria: 5,400
- Queensland: 4,600
- Western Australia: 2,000
- South Australia: 1,800
- Tasmania: 510
- Australian Capitol Territory: 370
- Northern Territory: 170
Click here to read the ‘Invisibility to Influence: Progress on MBC Data Reforms in Australia‘ report.
Prevalence of Breast Cancer in New Zealand
Breast Cancer is the most common cancer diagnosed in women in New Zealand. The prevalence of breast cancer has increased slightly over the past 20 years for both wāhine (female) Māori and non-Māori women, which researchers attribute to increased exposure and hormonal factors, as well as the expansion of the national breast screening program in 2004 to include women aged 45 – 69.
Breast Cancer Rates in Australia and New Zealand
Breast Cancer Incidence (Diagnosis) in Australia
In Australia, it is estimated that 20,440 people will be diagnosed with breast cancer this year or 56 people each day.
This number has significantly increased since records began. In 1983, 5,316 women and 61 men were diagnosed with breast cancer. This increasing incidence of breast cancer is thought to be due to a number of reasons including reproductive and hormonal factors, and improved screening and awareness.
While the average age of breast cancer is approximately 61 years, Cancer Australia has identified a trend in rising early onset cancers, including breast cancer. Between 2000 and 2025, the incidence of breast cancer in women aged 30–39 climbed from 22.1 to 22.7 cases per 100,000, and in the 40–49 age group, jumped from 76.6 to 81.1 per 100,000.
Breast cancer is the most commonly diagnosed cancer in Australia for persons aged 20 to 39 and persons aged 40 to 59.
Read more about why a growing number of women are being diagnosed with breast cancer.
Thanks to the Breast Screen Australia program, which invites women aged 50 to 74 to participate in free screening mammograms, it’s more likely breast cancer will be diagnosed at an early stage. This greatly increases a person’s chance of surviving their disease.
Breast Cancer Incidence (Diagnosis) in New Zealand
In New Zealand (Aotearoa), it’s estimated more than 3,600 new cases of breast cancer will be diagnosed this year or 9 poeple each day.
Breast Cancer Survival Rates in Australia and New Zealand
Survival Rates in Australia
In Australia, more people are surviving their breast cancer diagnosis than ever before. Thanks to the advancements made through clinical trials research, there are more tailored and advanced treatments, preventions, and screening techniques available.
However, for some people, their breast cancer will progress to an advanced or metastatic stage and this greatly reduces their chances of survival.
Your age and stage of disease has an impact on your chance of surviving five years past your breast cancer diagnosis. Those diagnosed with stage one breast cancer have an almost 100% chance of surviving five years post diagnosis, however those diagnosed with stage four breast cancer only have a 32% chance of surviving five years post diagnosis.
Overall, the five-year survival rate for women diagnosed with breast cancer is 93%, and 87% for men.
In 2025, it’s estimated that 3,300 women and 36 men will die from breast cancer in Australia.
Survival Rates in New Zealand
Breast cancer survival rates in New Zealand (Aotearoa) are improving. Most people diagnosed with breast cancer will now survive their disease. Although slightly lower than Australia’s survival rate, New Zealand’s (Aotearoa) rates are still positive with 89% of all women diagnosed with breast cancer surviving five years past their diagnosis. This has increased from 79% since 1999.
However, this rate doesn’t illustrate the reality for those with advanced or metastatic disease who, despite improved treatments can still die from the disease. It’s estimated that around 670 people will die from their breast cancer this year in New Zealand (Aotearoa), around 75 of these will be wāhine (female) Māori.
However, an evaluation of the national screening program Breast Screen Aotearoa from 1999 to 2011 found that participation in the screening program reduced mortality from breast cancer in women overall by 34%. This benefit was slightly lower in wāhine (female) Māori at 28%, but researchers say this discrepancy is due to lower numbers of wāhine (female) Māori participating in the program.
Breast Cancer Risk in Australia and New Zealand
Cancer Risk in Australia
A woman’s lifetime risk of being diagnosed with breast cancer in Australia is 1 in 7. For men it is 1 in 556. However, there are a number of ‘risk factors’ that can increaseor decrease this liklihood.
A risk factor is something about a person, or what that person is exposed to, that increases their chances of developing breast cancer in their lifetime. There are many different risk factors that can increase or decrease an individual’s personal risk of developing breast cancer. This includes genetic factors, such as an inherited genetic mutation like BRCA1 or BRCA2 or lifestyle factors such as alcohol, smoking, or lack of exercise. Although just because you have some risk factors does not mean you will be diagnosed with breast cancer.
Learn more about breast cancer risk factors.
You can assess your risk factors and their impact on your cancer risk using the iPrevent tool.
Cancer Risk in New Zealand
In New Zealand (Aotearoa), the risk of being diagnosed with breast cancer for women is 1 in 9.
It’s important women in New Zealand (Aotearoa) participate in regular breast screening every two years between the ages of 45 to 69 years. Participating in regular screening has been proven to reduce illness and death from breast cancer by detecting the disease early.
Learn more about clinical trials research, or find out more about our open clinical trials.



